Pregnancy related tummy gap

What is a tummy gap?
A Pregnancy-related tummy gap is called a diastasis rectus abdominis (DRA). It happens when the connective tissue strip down the mid-line of the abdomen, the linea alba, widens and thins to accommodate the growing baby. This natural physiological process has been reported to occur in 100% of pregnant women. The stretching also occurs on the entire abdominal wall as it contours around the expanding uterus. Rest assured, It is not a splitting of the muscle! After delivery, some women may notice a change in how their abdomen looks and feels. Some presentations may be related to the linea alba, some may be due to a relaxed abdominal wall, and some may be due to a combination of both. 66% of women have a DRA in their third trimester and 53% persists immediately post-partum (Boissonnault). 36% have DRA 8 weeks post delivery (Boissonnault). 100% of women have a DRA by 35 weeks gestation and the separation persists in 40% when measured at six months postpartum (Mota et al 2014).
There have been no mechanical factors found to cause a diastasis. It happens in women of all ethnicities, all ages, all heights, any body weight, any baby size and is not related to exercise. This leads us to think there could be more physiological factors but this has not yet been studied!
How do we measure it?
Mothers will notice doming of midline when lifting head off pillow or indenting and will be able to sink fingers in middle of abdomen. Normally an Ultrasound is useful to get a clear image but it is not always available in practices. Clinicians measure distances between left and right rectis abdominis by finger width but this can lead to different findings between practitioners.
What about the depth of the gap? The depth of the gap is just as important. Is there any resistance? Can my fingers keep sinking in? As you apply load to the abdominal wall (i.e: lifting head off pillow), there may be a change in the palpable depth of the linea alba.
The most important is actually the function of the rectus abdominis and not so much the inter recti distance. It is not about closing the gap but about function. Its about what happens to the tissue in the gap rather than the distance. The aim is to restore tension within that gap to promote better force transfer.

What can be done?
1/ Conservative treatment
It is a highly individual exercise based rehab/training. There are many ways to compensate for DRA and every patient has different habits, fitness goals and levels, occupation and therefore rehab should be personalised. Ultimately, trunk movements should not be avoided and there should be no limitations to exercise if its part of the patient’s goal. However, each exercise should be assessed to check whether the patient is ready or able to take on that task and then carefully and progressively reintegrated into the rehab program. The movement can be broken down into progressive elements to allow the patient to progress allowing them to gain strength and confidence in their abilities. For collagen to heal you have to load it. We can notice the linea alba thickening with training even though the gap distance might not change.
We want to support the patient and their rehab to progress towards their aims whatever they may be. Showing patients how to self monitor is key. Knowing when they are doing things right or when they are doing them in a less optimal way and how to correct themselves. How do you feel when doing the exercise, Do you feel strong?
Nowadays, There is a shift towards a more holistic approach to DRA management. Instead of focusing on closing or reducing the gap, clinicians are now aiming for control of the TA and other abdominal muscles during times of increased abdominal pressure (like a curl/ getting out of bed) to generate more tension on the linea alba and a better transfer of force, integrating the whole abdominal wall. You can feel a narrowing of the gap when doing a curl up without it generating tension through the midline tissues. Engaging the deep abdominal Muscles, like transversus abdominis (TA), in an efficient way could widen the gap but the distortion of the abdomen reduces. Even if initially in training the gap could widen, the women report reduced pain and doming, better function and they feel and look better.
2/ Surgical management:
Surgery is recommended when there is an 8,9,10 finger separation and the patient can not generate tension, there is doming and pain.
For the women in the middle range who have a 4-5cm gap it is very individual and dependant on who progresses and who doesn’t. 4-6 weeks of training should be attempted and if there are no changes or the patient is not able to recruit the abdominal wall and generate tension or control load through thorax and trunk, then surgery would be recommended. In any case, optimising function of abdominal wall and strengthening before surgery can not only eliminate some complications for surgeon but also allow a faster recovery due to motor memory of the muscles from the training.
How long will it take to recover?
As research evolves, exercises for DRA are becoming more progressive in nature, starting with connection-style exercises at the onset of rehab and progressing on to more global strengthening exercises for the large superficial muscles of the abdominal wall. Progress does not only mean reduction in gap. Clinicians consider and assess more the connective tissue integrity and function rather than the inter recti distance.
What is connective Tissue Integrity? The quality and thickness of the linea alba can improve depending on the loads placed on it. This can happen even as the size of the gap remains unchanged. It is important to be able to explain to the women why an increase in gap width is sometimes a sign of progression not regression. Therefore treatment and progress time frames need to adapt and follow the slower healing process of collagen. Connective tissue remodeling and rebuilding can take up to 2 years compared to weeks for muscular tissue.
66% of women with DRA have some pelvic floor dysfunction (urinary incontinence, constipation or pain with intercourse) 20-30 years postpartum compared to 6 months post partum when no correlation was found. So it’s not because symptoms are no present early in the post partum that they cannot develop down the line (due to various factors like repetitive compensatory mechanisms or further injury.)
In the practice, the aim would be for every women to have a post partum check for abdominal and pelvic floor and by 3 month basic function should be restored.
Post surgical management:
After 24 hours you are able to walk around even if you still have drains and compression garments. The healing of incision takes around 3 weeks but the patient is still in moderate amount of pain for another 2 weeks. After 5 weeks training can begin again by waking up and connection to the abdominal wall system and to get a sense of feedback. After 7-8 weeks, movement can be introduced to the rehab program. By 3 Months onward the healing is done and aims can be reached!
What can hinder progress?
The main factors that can hinder progress are:
Posture: poor body mechanics leading to suboptimal recruitment of muscles and compensations and leading to increased intra abdominal pressure. Intra abdominal pressure is always present but the level can change depending on your activity i.e coughing, laughing, pooing, breathing, moving etc.. if you imagine your two hands wrapped around a balloon like your abdominal wall around your guts then you can see how squeezing your hands together can increase the pressure in the balloon. Now consider that you are 3 stacked ballons (thoracic, abdominal and pelvic) so one ballon can affect the other!

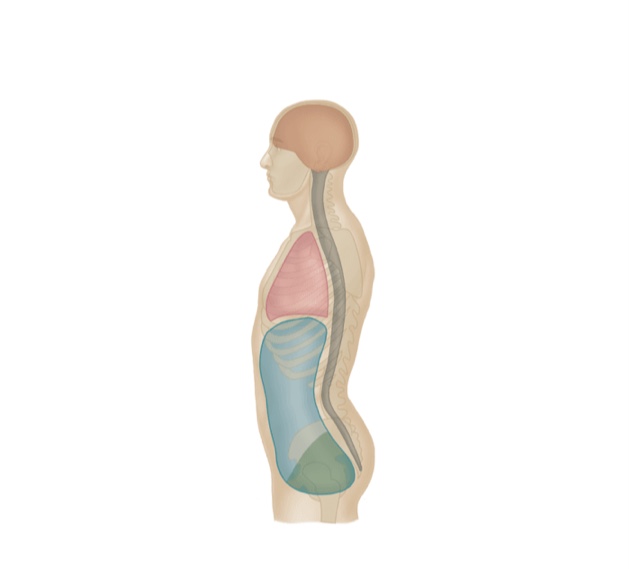
Breathing: breathing is such an essential and automatic part of our lives that we forget to pay attention to it. However breathing mechanics are crucial to our body not only on a cellular level but for our posture and ability to exercise and move. If you go back to the ballon imagery in the previous paragraph you can see how holding you breath or only breathing from the chest could affect the pressure in your abdominal wall and therefore function of you muscles. Breathing out naturally creates a contraction of your deep abdominal muscles therefore it cannot be ignored in your rehab process!
Diet/gut health: foods that cause inflammation and swell the abdomen like with intolerances and allergies. We know that there is a reflex inhibition of the abdominal wall in response to visceral inflammation. This means there is difficulty engaging the abdominal wall when your tummy is upset! Maybe this is where future research could help diastasis management by looking at the response of the tissues on a physiological and nutritional level…
Should I have avoided certain exercise during pregnancy?
Training and exercise is totally fine for an uncomplicated healthy pregnancy. We can not predict who will have a sustained or a wider DRA after birth. There are more benefits of exercise than risks. It is generally advised to avoid starting a new type of exercise but otherwise continuing what you have been doing is good. It is about listening to your body as you go through pregnancy and adapt to your fatigue and body changes. In the last trimester and especially in the last 6 weeks of pregnancy, exercise can become more tricky simply because your baby is taking more space and breathing becomes more demanding. There is a widening of your intercostal angle (can go ip to 35o!) to accommodate your baby and the shift of organs, therefore there is less support for diaphragm. So you will have to adapt the intensity or nature of your exercise to cope with these changes.
Conclusion:
DRA is not just about the tummy gap but about function of the whole abdominal wall. Any women can get post natal DRA so there’s nothing you did wrong or bad! There is unfortunately no quick fix or magic recipe and the aesthetic aspect of DRA might not alway be resolved. The treatment and management of DRA has become much more holistic and as therapists we are here to help you strengthen and achieve your goals no matter what they are. Reintegration of exercises is done progressively and safely and is individual to the women’s needs and abilities. We work on both visible and invisible parts of your body that need to work together to allow your abdominal muscles to work optimally and there is a lot that can be done to help resolve symptoms and strengthen. There is still a lot we do not know about DRA and hopefully research will answer more questions for us in the future. We have to grow and adapt our practice and help our patient the best we can with the information we have. DRA and pelvic floor post natal check should be accessible to every women. Hopefully, treatment and management of DRA will become more widely covered and surgical intervention will no longer be considered as cosmetic.
More information can be found here with ultrasound imagery:
https://babybellypelvicsupport.com/diastasis-rectus-abdominis/ https://dianeleephysio.com/education/diastasis-rectus-abdominis-postpartum-health/
Suggested read for understanding DRA and for postural to global exercises : diastasis recti by Katy bowman
Specialists: Munira Hudani/ Diane Lee/ Graine Donnelly/ The mummy MOT

